

Do you wake up every morning with blurry vision before fumbling to find your glasses or putting in your contact lenses? Do you ever wonder what it would be like to wake up and be able to see the world around you with clarity?
For those that qualify, procedures like LASIK and PRK can be life-changing ways to say goodbye to glasses and contacts for good.
LASIK is a procedure that corrects refractive errors like nearsightedness, farsightedness, and astigmatism. LASIK works by reshaping corneal tissue using a laser for the most precision.
LASIK is a popular elective procedure that corrects vision for many patients to 20/20 or better. Most people that have LASIK are able to go through life without needing their glasses or contacts to see.
Like any surgical procedure, LASIK is not for everyone. To undergo this procedure, you must first qualify as a candidate.
There are many factors that go into LASIK candidacy. Some of the most common include:
To get LASIK, you need to be at least 21 years old. If you get LASIK when you’re younger, there’s a good chance that your eyes will continue changing after you have the procedure.
You should not get LASIK if your eyes are unhealthy. If you have any conditions like cataracts, glaucoma, retinal disease or severe dry eye syndrome, you will not be a good candidate for the procedure.
When you’re pregnant or nursing, there are hormonal changes happening constantly. Your eyes are even affected by this, meaning your prescription may change.
Becauseof the increase of hormones in your system. you shouldn’t have LASIK until at least 3 months after you’ve stopped nursing. This will help to ensure that your prescription has stabilized and you have the best outcome possible.
Another important factor for LASIK candidacy is having a stable prescription. At an absolute minimum, your prescription needs to remain unchanged for 1 year, if not longer.
If your eyes are still changing, wait before having LASIK.
You must be in good health to undergo LASIK. This doesn’t mean you need to be perfectly healthy, but you can’t have any autoimmune conditions like Sjogren’s syndrome, HIV, or diabetes. These conditions affect how your body heals after any procedure.
Sufficient Corneal Thickness During your LASIK consultation, one of the things that are measured is the thickness of your corneas. You must have thick enough corneas to safely have LASIK.
A tiny amount of corneal tissue gets removed during the procedure to correct your vision. If your corneas are too thin, removing even a small amount of tissue may lead to complications.
These are only some of the factors that go into LASIK candidacy. To know for sure if you are a good LASIK candidate, schedule a LASIK consultation at Colorado Eye Consultants in Littleton!
LASIK is an outpatient procedure, meaning you can go home the same day. Before the procedure starts, you’ll receive numbing eye drops.
Once the eye is numb, your doctor will then use a laser to create a flap on the cornea. The laser then gently reshapes the corneal tissue according to your prescription. Nearsightedness, farsightedness, and astigmatism can all be corrected with LASIK
After completing the corneal reshaping, the flap is repositioned and left to heal in place without the need for stitches or sutures. LASIK generally takes approximately 15 to 20 minutes to complete. After you’re cleared by your surgeon, you can go home and begin recovering with your beautiful new vision!
The recovery after LASIK is one of the shortest for a refractive procedure. You may notice that your vision is already improved right after LASIK or it may take a few days.
Both are normal! You cannot drive yourself home so make sure you have someone that can drive you on the day of your procedure.
Once you’re home, one of the best things you can do is sleep. You’ll need to wear an eye shield that protects the delicate flap for the first 24 hours after LASIK.
You’ll need to continue wearing this shield for two weeks after your LASIK procedure at bedtime. This prevents any bumping or rubbing that may occur while you’re sleeping.
You may experience some slight discomfort such as your eye feeling irritated, scratchy or a burning sensation, over-the-counter pain relievers and artificial tears can help with this.
Once your eye doctor clears you, you can resume driving. Many people return to work the day after LASIK, but it’s recommended to take 2-3 days off to rest.
You’ll need to avoid activities like exercising, swimming, contact sports, and wearing eye makeup for at least a week to a month after LASIK. Check with your eye doctor to determine when you can return to certain activities.
Your vision will continue to improve after LASIK as your eye heals. Most patients end up with 20/20 vision or better once their eye is fully healed.
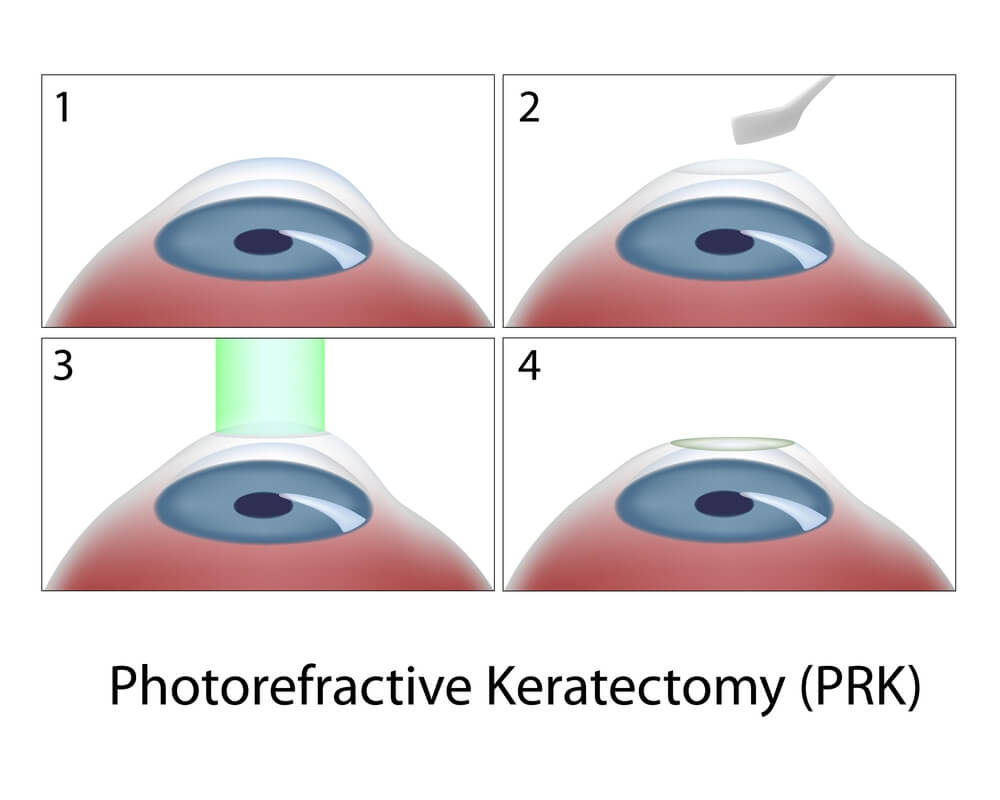
Another option for vision correction is a procedure called PRK. PRK is a procedure that can also correct nearsightedness, farsightedness, and astigmatism.
PRK stands for Photorefractive keratectomy. It permanently changes the shape of the cornea while improving how light focuses on the retina, allowing for clear vision without the dependence on glasses or contact lenses.
PRK may be a good option for people who are not good candidates for LASIK, especially if their corneas are too thin. During PRK surgery, the outer cell layer of the cornea (called the epithelium) is removed.
An excimer laser then gently reshapes the cornea. Unlike LASIK, there is no flap created during PRK.
This is what makes it ideal for patients with thinner corneas. PRK is an outpatient procedure that takes around 10 to 15 minutes to complete. Your surgeon will numb your eyes with numbing drops and use an eyelid holder to keep your eyes open during the procedure.
Immediately after PRK, you’ll have a bandage contact lens placed on your eye for protection. This will also reduce any discomfort while you heal from the procedure.
Patients may feel some discomfort the first few days after surgery and your vision may be blurry for a few days to several weeks. Your doctor will prescribe eye drops and pain medication to use during the healing process.
You will notice an improvement in your vision within the first week, but it may take a month or longer before you experience your best vision. PRK patients have a longer period of healing than LASIK patients.
Although it’s a longer recovery period, PRK is the preferred method of eye surgery for patients with thin corneas or large pupils.
To know if PRK is right for you, schedule a consultation at Colorado Eye Consultants.
The best candidates for PRK are:
Our board-certified surgeons at Colorado Eye Consultants have performed countless LASIK and PRK procedures. They can advise you on what treatment will work best for your eyes.
Schedule a consultation at Colorado Eye Consultants in Littleton, CO to see if you are a candidate today!
Colorado Eye Consultants is dedicated to the preservation of sight and providing patients with the quality of life they deserve. Our patients receive personalized care by knowledgeable and experienced board certified ophthalmologists to ensure the clarity needed to see the most important things in their world. Your vision is our utmost priority and we offer same day appointments to ensure you get the care you deserve!
Request an Appointment