
Are you or a loved one concerned about a recent diagnosis of glaucoma? The ophthalmologists at Colorado Eye Consultants are well-versed when it comes to treating glaucoma.
Glaucoma is an eye condition that damages the nerve in the back of the eye called the optic nerve. The optic nerve is an important part of the eye that sends messages to the brain.
This allows light that passes through the eye to be converted into images. If the optic nerve suffers any damage, it affects our vision. The symptoms can start so slowly that you don’t even notice them. More than half of people with Glaucoma don’t even know they have it. Over time, you may slowly lose vision which usually starts in the peripheral part of your vision. As the disease progresses you may start to notice you can’t see things to the side. Without treatment, glaucoma can eventually cause blindness.
There are many different types of Glaucoma, but the most common form of glaucoma is open-angle glaucoma. Other types of less common are angle-closure glaucoma and congenital glaucoma
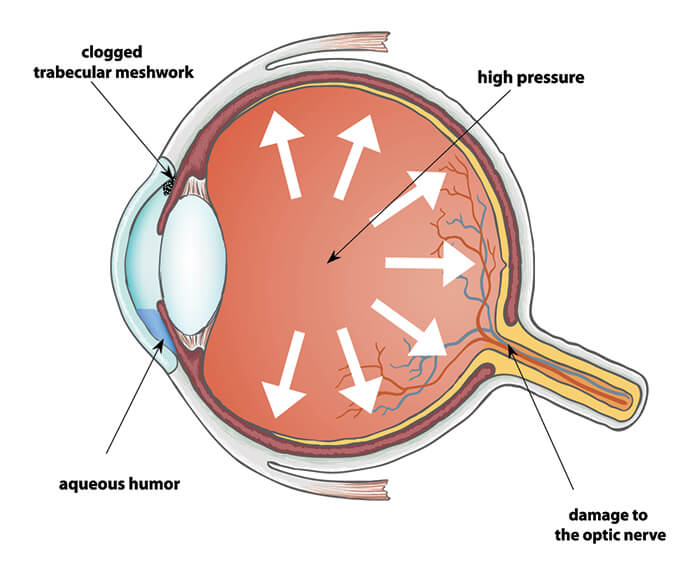
Open-angle glaucoma develops when pressure builds and blocks the trabecular meshwork. This is the tissue that allows the eye to drain fluids.
This kind of glaucoma happens slowly. There are no symptoms until the optic nerve is already damaged.
This results in gradual vision loss. That is why it’s important for patients to have regular eye exams to check their eye pressure.
There are several factors that can put you at risk for glaucoma. The primary one is age.
Glaucoma is one of the leading causes of blindness in people who are 60 and older. There are other factors that increase your risk for developing glaucoma earlier. These include:
If you know you’re at risk for glaucoma, it’s important to have regular eye exams. This is the only way your eye doctor can diagnose glaucoma in the early stages.
There is no cure for glaucoma, but if it’s found early, it is manageable. When it’s managed properly, the progression of vision loss can be slowed down.
Initial therapy for glaucoma usually consists of eye drops or laser treatment. However, advancements in technology have allowed for more options available to treat and manage mild to severe glaucoma and have proven to be more effective than ever before.
There are a lot of options available when it comes to glaucoma treatment. Those options include:
Innovation in eye care has led to the invention of Micro invasive Glaucoma Surgery “MIGS”. Historically when medication and laser therapy have failed to control a patient’s IOP, incisional surgery was required. Despite their efficacy, these procedures came with higher risks and rates of complications. Because of this, it was generally reserved for patients with severe glaucoma. For many years, doctors were left with gaps in treatment for patients with mild to moderate glaucoma who had uncontrolled IOP despite pharmaceutical and laser therapy. Advancement in the field of Glaucoma led to the advent of MIGS, which sought to fulfill the unmet needs in treatment options and close the gap.
MIGS can treat mild to moderate glaucoma and are a great option when other treatments have failed, or a patient is intolerant or non-compliant with medications. There are many classifications of MIGS that target various aspects of the normal aqueous dynamics.
Let our board-certified ophthalmologists help find the best option for you.
Schedule an appointment with the eye doctors at Colorado Eye Consultants to learn more!
Colorado Eye Consultants is dedicated to the preservation of sight and providing patients with the quality of life they deserve. Our patients receive personalized care by knowledgeable and experienced board certified ophthalmologists to ensure the clarity needed to see the most important things in their world. Your vision is our utmost priority and we offer same day appointments to ensure you get the care you deserve!
Request an Appointment