
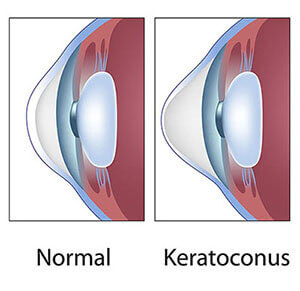
Keratoconus is a degenerative disorder of the eye in which the normal round shape of the cornea thins and develops a cone-like bulge. Often appearing in the teens and early twenties, the disease can cause significant visual impairment, including distorted and blurred vision and corneal scarring. Progression of the disease generally occurs gradually and can slow or stop at various stages, leaving a range of impairment from mild to severe.
The exact cause of keratoconus is not known, although a number of scientific theories point to a combination of factors including genetics, environmental and cellular causes.
According to the National Keratoconus Foundation, approximately one out of every 2,000 people will develop this condition. Most cases of keratoconus appear to start spontaneously, however, approximately 14% of new cases present with evidence of a genetic link. Because the onset of the disease generally starts during puberty, some scientists are studying a possible link to the endocrine system. Other commonly recognized risk factors include excessive eye rubbing, a history of rigid contact lens wear and the presence of one or more atopic diseases such as asthma and eczema. People with Down syndrome are also more likely than the general population to develop keratoconus.
The first sign of keratoconus is blurred or distorted vision. In the early stages of the disease, patients often experience progressive worsening of nearsightedness and astigmatism and require frequent eyeglass prescriptions changes in order to improve vision. The continued thinning of the cornea progresses slowly, sometimes over a period of 10-20 years, before slowing or stopping.
On occasion, if progression is rapid and keratoconus moves into the advanced stage, patients can develop hydrops, a clouding of vision in one eye. Hydrops is caused by a sudden infusion of fluid into the stretched cornea, making the cornea appear swollen and opaque. It is a rare complication that gradually clears over several weeks or months, although in severe cases, the central part of the corneal bulge can form superficial scarring and further impair vision.
In the early stages of keratoconus, mild myopia (nearsightedness) and astigmatism are corrected with eyeglasses or contacts. As the condition progresses, rigid gas permeable (RGP) contact lenses are prescribed to be better manage the distorted vision caused by increased astigmatism.
Another treatment option is Intacs. Approved by the FDA in 2004, Intacs are tiny plastic inserts that are placed in the periphery of the cornea to help re-shape the cornea and improve vision.
Corneal collagen crosslinking is an option recently approved by the FDA. It involves absorbing specially prepared riboflavin eye drops into the cornea and utilizing ultraviolet light to create a biochemical reaction to strengthen the cornea and make it more rigid. This serves to halt the progression of keratoconus preventing it from worsening. It is not meant as a procedure to improve the cornea shape and focus of the eye. This will still require glasses or likely a contact lens.
If none of the available treatment options work, or the disease progresses to an advanced stage, then a corneal transplant may become necessary.
To address the visual distortion created by keratoconus, rigid gas permeable (RGP) lenses are often used in treatment. These lenses are ideal for a number of reasons:
Other forms of contact lens treatment are also available to treat keratoconus, including: custom soft contact lenses, hybrid contact lenses,”piggyback” lenses and large scleral lenses.
Colorado Eye Consultants is dedicated to the preservation of sight and providing patients with the quality of life they deserve. Our patients receive personalized care by knowledgeable and experienced board certified ophthalmologists to ensure the clarity needed to see the most important things in their world. Your vision is our utmost priority and we offer same day appointments to ensure you get the care you deserve!
Request an Appointment